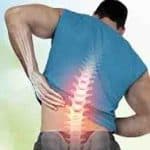
ISLAMABAD, April 05 (online): Researchers in China and the U.S. have found that chronic musculoskeletal pain (CMP) could be linked to a higher risk of brain aging and dementia.People with knee osteoarthritis were found to have more rapid brain aging than people without it.A genetic link between inflammation and brain function may point toward a way to predict cognitive decline, but further study is needed, experts say.
Chronic musculoskeletal pain (CMP) may contribute to a higher risk of cognitive decline, according to a new study by scientists from the U.S. and China.The study, published in Nature Mental HealthTrusted Source, examined the MRI data from more than 9,000 people in the United Kingdom and discovered a connection between knee osteoarthritis (KOA) and accelerated brain aging.
With slightly less than halfTrusted Source of the global population experiencing CMP, the study provides a window for researchers into how inflammation and cognitive function can be linked and studied in the future. CMP’s role in accelerated cognitive decline has not been extensively studied, but many older adults who experience it are at greater risk for dementia.
Researchers developed a comparative model using structural MRI data that allowed them to examine the differences between brain age and chronological age.
They found that people with KOA had much more rapid brain aging than those without it.
How does chronic musculoskeletal pain affect the brain?
Inflammation in the body has been seen as a contributing factor to neurological ailments, Steve Allder, MD, consultant neurologist at Re:Cognition Health, who was not involved in the study, told Medical News Today.
“Increasingly, particularly for depression and Alzheimer’s, and other conditions — for example, a recent reviewTrusted Source invoked this in Parkinson’s disease, traumatic brain injury, Amyotrophic lateral sclerosis, Gulf War Illness, and myalgic encephalomyelitis/chronic fatigue syndrome,” Allder said.
Medhat Mikhael, MD, pain management specialist and medical director of the non-operative program at the Spine Health Center at MemorialCare Orange Coast Medical Center in Fountain Valley, CA, who was also not involved in the study, told MNT that inflammation and chronic pain can interrupt and alter the brain’s processing patterns.
“Chronic inflammation like knee Osteoarthritis or Chronic Musculoskeletal pain are associated with changes in the central nervous system causing what is known as neuroplasticity, which changes in the structural and functional state of the brain,” Mikhael said. “Chronic pain (CP) has been found to cause significant alternations of the brain’s structure and function due to changes in pain processing and disrupted cognitive functions, including with respect to the prefrontal cortex.”
The inflammation that stems from acute pain can become chronic if not properly addressed, but in general, an injury to one particular area is not likely to cause cognitive decline, according to Allder.
“You need to provoke a sustained immune response both systematically and in the brain,” Allder said.
Linking chronic pain and cognitive decline
The new study suggests that the gene SLC39A8Trusted Source, which is expressed in microglial cells and astrocytes, is the connection between KOA and cognitive decline. Mikhael explained that SLC39A8 encodes the protein ZIP8, which transports essential metals like ferrum, manganese, and zinc, and the nonessential neurotoxic metal cadmium.
“Genetic mutations may affect the transport and uptake of essential metals to the mitochondria, particularly the manganese, which seems to be essential for the health and function of the brain cells,” Mikhael said. “Excess metal exposure or toxic effect can have major negative side effects.”
Allder pointed to a large number of other health issues that are linked to SLC39A8, including:
“clinical disorders in virtually every organ, tissue, and cell type: numerous developmental and congenital disorders, the immune system, cardiovascular system, kidney, lung, liver, coagulation system, central nervous system, musculoskeletal system, eye, and gastrointestinal tract,” he said.
He added that the study should provoke further understanding of the links between CMP and cognitive decline, but also of the wide variety of problems that can arise from the gene’s imbalance.
“Traits with which SLC39A8-deficiency variants are currently associatedTrusted Source include Mn2+-deficient hypoglycosylation; [n]umerous birth defects; decreased serum high-density lipoprotein-cholesterol levels; increased body mass index; greater risk of coronary artery disease, hypotension, cardiovascular death, and Parkinson’s diseas[e],” among many others, Allder said.
Mikhael said one drawback to the study is that the focus from the data became too narrow for studying such a significant cognitive drop, since it was primarily about chronic knee pain and the path to brain aging related to SLC39A8.
“It would have been beneficial to study other chronic inflammatory pain disorders and see if they would come to the same conclusion,” Mikhael said.
In Conversation: How to understand chronic pain
Chronic pain, a disease process that is so complex that we are only just beginning to understand its triggers, has recently been gaining recognition as a medical condition on its own. But how does living with chronic pain feel? And how do the body and brain deal with it?
Design by Andrew Nguyen
Aching, dull, gnawing, burning, sharp, shooting, piercing…
These are just some of the words people tend to use to describe their pain.
Now imagine you had to endure a bit of this every waking day until you don’t know what it’s like to go about your day without this baseline of pain slowly depleting your mental and physical energy in the background.
That is the reality for many people who deal with chronic pain.
Some days may be great, some days bad; the signs may not always be visible and it may be an inward battle hidden behind gritted teeth and forced smiles.
But how does chronic pain become, well, chronic?
Follow the PNI Facebook page for the latest news and updates.